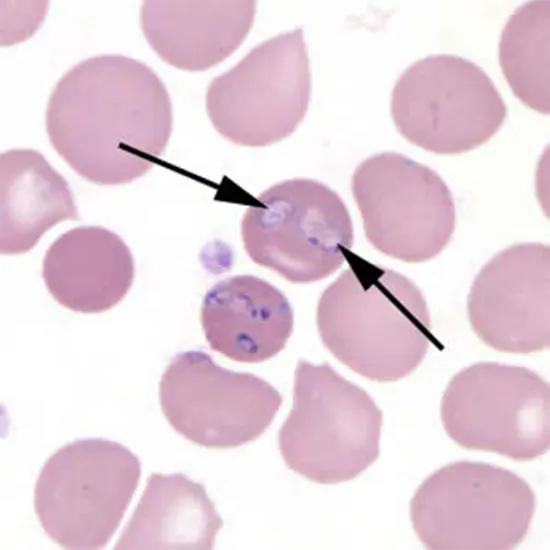
A family of parasitic protozoa known as babesia invade red blood cells and cause a variety of illnesses in both people and animals. Babesia, which has more than 100 different species, is spread by ticks and other arthropods...
A family of parasitic protozoa known as babesia invade red blood cells and cause a variety of illnesses in both people and animals. Babesia, which has more than 100 different species, is spread by ticks and other arthropods that feed on blood. Babesia infections can result in a wide range of symptoms, from minor flu-like symptoms to serious and possibly fatal illnesses.
Animals with both domesticated and wild mammals, such as cattle, horses, dogs, and deer, frequently contract Babesia infections. Depending on the species of Babesia and the host animal, the illness known as Babesiosis, which is brought on by a Babesia infection, can cause anemia, fever, weakness, and other symptoms.
Babesia infections in people are very uncommon, but they can be dangerous, especially in those with compromised immune systems. The most prevalent types of Babesia that affect people are Babesia microti and Babesia duncani, both of which are spread by ticks. Babesiosis in people can manifest as symptoms including fever, exhaustion, aches in the muscles, and anemia.
What Can Be The Classification?
A genus of parasitic protozoa in the phylum Apicomplexa is called Babesia. The host range, vector(s), and genetic traits of the species in the genus are used to further categorize them. Important Babesia species and their classification include:
Babesia microtia:
- Host range: Humans, rodents, and other small mammals
- Vector: Ixodes scapularis tick
- Classification: Babesia microti complex
Babesia divergens:
- Host range: Cattle
- Vector: Ixodes ricinus tick
- Classification: Babesia divergens complex
Babesia bigemina:
- Host range: Cattle
- Vector: Boophilus tick
- Classification: Babesia bigemina complex
Babesia bovis:
- Host range: Cattle
- Vector: Boophilus tick
- Classification: Babesia bovis complex
Babesia canis:
- Host range: Dogs
- Vector: Dermacentor reticulatus tick
- Classification: Babesia canis complex
Babesia senator:
- Host range: Humans, deer, and other wild mammals
- Vector: Ixodes ricinus tick
- Classification: Babesia Sanatorium complex
Babesia duncani:
- Host range: Humans
- Vector: Ixodes pacificus tick
- Classification: Babesia Duncani complex
Babesia Genetics: Unlocking The Secrets Of A Deadly Parasite.
Single-celled parasites called Babesia species are members of the phylum Apicomplexa. They have a complicated life cycle that involves interactions with their host and vector at several developmental phases. Babesia species' biology, epidemiology, and pathology are significantly influenced by their genetics.
In comparison to other Apicomplexa parasites, Babesia species have relatively tiny genomes, with sizes between 6 and 8 megabases. They have a single set of chromosomes and a haploid genome that is extremely compact and has few non-coding regions. In addition to genes that are exclusive to Babesia and are engaged in parasite-host interactions, the genomes of Babesia species also contain genes involved in signal transduction, transcriptional control, and metabolism.
The babesia species have a very diverse genetic makeup, with many genetic strains or variants existing within each species. The enormous rates of mutation, genetic recombination, and gene conversion that occur throughout the parasites' sexual and asexual reproduction are the cause of this genetic diversity. The genetic diversity of Babesia species and their vectors is also influenced by their geographic distribution.
The epidemiology and pathophysiology of Babesia species are significantly impacted by genetic variation. For instance, genetic variations across Babesia strains may have an impact on the parasite's host range and pathogenicity. Certain Babesia strains are more virulent than others and have a wider host range. Genetic variations can also alter how the parasite responds to medication and immune evasion tactics, as well as how it is transmitted by its vector.
Babesia genetics can now be studied at a deeper level thanks to improvements in sequencing technologies and genetic tools. This has allowed researchers to learn more about the biology and evolution of these parasites. For the creation of new diagnostic tools, medications, and vaccines as well as for the development of successful babesiosis control measures, it is essential to comprehend the genetics of Babesia species.
Babesia Transmission Dynamics: From Ticks To Hosts And Back.
Animals and people can contract babesia species from infected tick bites. By consuming infected animals, such as rats, deer, and other mammals, ticks pick up Babesia parasites. Ticks can carry the disease for the duration of their life, which can be anywhere from a few months to several years after they become infected.
Babesia is transmitted while a tick is eaten. When an infected tick bites a host, it injects the Babesia parasites into the host's skin through its saliva. The parasites then infect red blood cells in the host's bloodstream, reproduce there, and spread disease.
All phases of tick development, including the larval, nymphal, and adult stages, are susceptible to babesia transmission. The danger of transmission is greatest, however, while the tick is in its nymphal stage, which is when it feeds most frequently on people and animals.
Ticks of the Ixodes genus, which are present in temperate zones all over the world, including North America, Europe, and Asia, are most frequently linked to the transmission of the babesia virus. Babesia microtia and Babesia duncani, which are spread by the black-legged tick (Ixodes scapularis) and the western black-legged tick (Ixodes pacificus), respectively, are the two most prevalent Babesia species that infect people in the United States.
Babesia Life Cycle: A Complex Journey From Tick To Host And Back.
Babesia species have a complicated life cycle that includes a mammalian host in addition to a tick as the vector. A general summary of the Babesia life cycle is provided below:
Infection of tick vector: Babesia parasites start their life cycle when they are consumed by a tick during a blood meal, which is how the tick vector becomes infected. All tick life stages, including larvae, nymphs, and adults, are susceptible to parasites.
Parasite migration and multiplication: While inside the tick's digestive tract, Babesia parasites multiply and divide to generate the sporozoites, merozoites, and gametocytes stages. When the tick next feeds, the parasites move to the tick's salivary glands, where they can infect the mammalian host.
Mammalian host transmission: When a tick feeds on a mammalian host, the tick injects Babesia parasites into the host's skin through its saliva. The parasites then invade red blood cells after entering the bloodstream, where they continue to grow and spread disease.
Multiplication and spread within the host: Babesia parasites continue to grow and penetrate new red blood cells inside the host, where they continue to replicate asexually. Anemia and other issues might result from the parasites' severe red blood cell destruction as they reproduce.
Sexual reproduction and transmission to tick: Certain Babesia parasites also engage in sexual reproduction inside their mammalian hosts, creating male and female gametocytes, which can then be transmitted to ticks. The gametocytes are consumed along with the host's blood when an infected tick feeds on the host once again. The gametocytes combine to create zygotes, which develop into sporozoites and move to the salivary glands, in the tick's gut. When the infected tick feeds on a fresh host, the cycle starts over.
What Can Be the Signs and Symptoms?
Flu-like symptoms include fever, chills, exhaustion, headaches, and muscular aches, which are common in persons with Babesia infections.
Babesia parasites can destroy red blood cells, which results in anemia (low red blood cell count). Weakness, exhaustion, shortness of breath, pale complexion, and a quick heartbeat are all possible anemia symptoms.
Rarely, a severe Babesia infection can result in hemolytic uremic syndrome (HUS), a hazardous illness that can lead to renal failure, anemia, and a low platelet count.
What Can Be The Diagnosis And Treatment Plan?
Diagnosis
Blood tests: Blood tests may be done to find Babesia parasites in the patient's blood. These tests can include serological tests that look for parasite antibodies as well as microscopic examination of a blood smear, cbc, lft, kft, ldh and Babesia Microti Antibodies IgG and IgM to look for parasites and confirm the presence of antibodies.
PCR testing: Babesia DNA can be found in blood samples using polymerase chain reaction (PCR) testing, leading to a more precise and sensitive diagnosis.
Imaging testing: In some cases to diagnose the affect of spread of infection to other parts of body and its severity, doctor may ask for chest x ray scan.
Treatment
Babesia infection is typically treated with antiparasitic drugs, such as atovaquone and azithromycin or clindamycin and quinine. These drugs can aid in the removal of parasites from the blood and stop future harm.
Supporting care: When Babesia infection is severe, supportive care may be required, including blood transfusions to treat anemia and intravenous fluids to assist patients to stay hydrated.
Babesia infection can be avoided with prevention. This can involve staying away from tick bites, donning protective gear, applying insect repellent, and routinely checking for ticks when spending time outside.
A significant group of parasitic protozoa known as the Babesia species can seriously Allen both people and animals. Babesia infections can be difficult to diagnose and treat, but early medical intervention and tick bite avoidance strategies can significantly lower the risk of serious illness. It is critical to seek medical help right away if you believe you may have been bitten by a tick or exposed to Babesia to receive a thorough diagnosis and course of therapy.
















