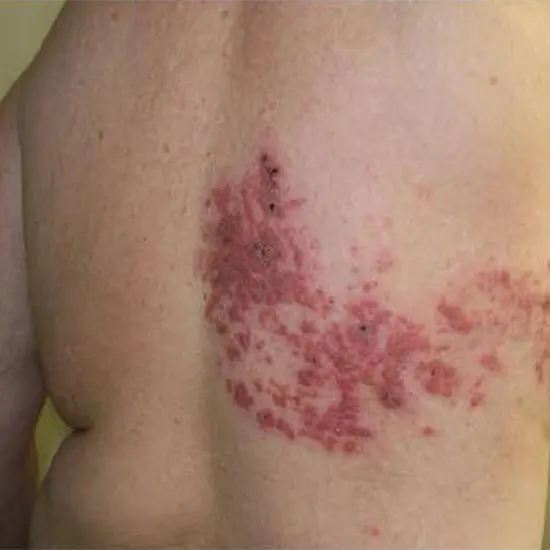
Shingles is commonly known as herpes zoster. It is a viral illness brought on by the varicella-zoster virus reactivating in the sensory or spinal ganglia of cranial nerves following a prior chicken pox infection.
Shingles is commonly known as herpes zoster. It is a viral illness brought on by the varicella-zoster virus reactivating in the sensory or spinal ganglia of cranial nerves following a prior chicken pox infection. Chickenpox is commonly known as chickenpox. Shingles occurs in adults or the elderly, but occurs in children.
Shingles is thought to result from a failure of the immune system that controls latent replication of the virus. Herpes zoster incidence and immunological function are closely connected.
Shingles rarely appear in those who have high immunity levels. Infections are not benign and can manifest in many ways. Even after the shingles have healed, many individuals still have moderate to severe pain, often known as postherpetic neuralgia.
Etiology
Upon reactivation, the virus replicates in the nerve cell body and virions are released from the cell and carried down the nerve to areas of the skin innervated by this ganglion. On the skin, the virus causes local inflammation and blisters. Pain from shingles is due to viral nerve inflammation.
Triggers for shingles include:
- Mental stress.
- Taking drugs (immunosuppressants).
- Acute or chronic illness.
- Exposure to viruses.
- Presence of malignant tumor.
Epidemiology
In young, healthy people, the incidence of herpes zoster ranges from 1.2 to 3.4 per 1000 people per year, while it ranges from 3.9 to 11.8 per 1000 people per year in patients 65 years of age and beyond. Shingles do not vary according to the season.
Relapses are most common in immunocompromised patients.
Pathophysiology
Herpes zoster skin lesions induce varicella-zoster virus-specific T-cell proliferation, whereas interferon-alpha production leads to herpes zoster resolution. Immunocompetent patients have particular antibodies (IgG, IgM, and IgA) that are resistant to the varicella-zoster virus because they develop more quickly and at higher titers after reactivation (herpes zoster). Long-lasting enhanced cell-mediated immunity is provided.
Dermatological involvement is afferent and follows the dermatome. The lumbar and cervical spine are most often involved, but movements are rarely involved. The infection is contagious to people who do not have previous immunity to varicella zoster, but transmission rates are low. The virus is transmitted by direct skin contact or by inhaling infected droplets.
It is important to know that herpes infections can also occur at the same time. Herpes simplex, CMV, EBV, and human herpes virus have all been found in patients with shingles.
History and Physical
Shingles is characterized by a prodrome of fever, malaise, and excruciating burning pain, followed by vesicular eruptions over 3-5 days with 1-3 harvests. Lesions are unilaterally distributed within a single dermatome.
Clinically, the lesions begin as dense erythematous papules that rapidly become vesicular on an erythematous and edematous basis and can be contiguous or discontinuous in one, two, or more MRI Myelography adjacent dermatomes. It can occur unilaterally in the band. Commonly affected dermatomes are thoracic (53%), cervical (20%), and trigeminal (15%), including ophthalmologic and lumbosacral (11%).
The three stages of infection are:
During the pre-eruption stage, abnormal cutaneous sensation or pain is seen within the affected dermatome. This stage occurs at least 48 hours before overt lesions. At the same time, they may suffer from headaches, general malaise, and photophobia.
The acute eruptive phase is characterized by vesicle formation and pre-eruptive phase symptoms. Lesions first start out as CSF Examination Routine patches that quickly turn into painful blisters. Blisters often rupture, suppurate, and eventually crust over. Patients are most contagious at this stage until the lesion dries.
Traditional painkillers frequently don't work at this point since the pain is so acute. This stage he may last 2-4 weeks, but the pain may persist.
Chronic infections are characterized by recurrent pain lasting 4 weeks or longer. In addition to pain, patients Giemsa Stain experience paresthesias, shock-like sensations, and paresthesias. The pain is incapacitating and can last 12 months or longer.
Shingles is also known as Ramsay Hunt syndrome type II. This is because the virus spreads from the facial nerve to the vestibulocochlear nerve, affecting the ear and causing hearing loss and dizziness (vertigo).
Shingles can occur in the mouth when the maxillary or mandibular portion of the trigeminal nerve is affected. Clinically, it presents as vesicles or erosions that appear on the mucosa of the maxilla (palate, gums of upper teeth) or mandible (tongue or gums of lower teeth). Oral lesions may occur alone or in combination with skin lesions overlying the same trigeminal branch cutaneous distribution.
Viruses can spread to blood vessels because of the tight connection between blood vessels and nerves, which might alter blood flow and result in ischemia necrosis.
This can lead to complications such as osteonecrosis, tooth loss, periodontitis, pulpal calcification, pulpal necrosis, periapical lesions, and abnormal tooth development.The ocular part of the trigeminal nerve is the most commonly affected branch that causes ocular herpes.
The skin of the forehead, upper eyelids, and eye sockets may be affected. It is seen in approximately 10% to 25% of cases with features of keratitis, uveitis, and optic paralysis. Complications can occur in the form of chronic eye inflammation, vision loss, and debilitating pain.
CNS involvement is not uncommon. Because the virus resides in sensory root ganglia, it can infect any part of the brain, causing cranial nerve palsies, muscle weakness, diaphragmatic palsy, neurogenic bladder, Guillain-Barré syndrome, and myelitis. Patients may acquire encephalitis in severe situations.
Secondary bacterial infections, postherpetic neuralgia, scarring, nerve paralysis, and, in situations of widespread shingles, encephalitis are among the complications of shingles.
Herpes zoster disseminated is defined as more than 20 skin lesions occurring primarily outside the affected area or immediately adjacent dermatomes. Organs other than the skin can also be affected, causing hepatitis and encephalitis, a condition that can be fatal.
Postherpetic neuralgia is a condition in which pain persists one month after the onset of herpes zoster. This is the most common side effect seen in older patients involving the ocular part of the trigeminal nerve.
Complications such as cranial neuropathy, polyneuritis, myelitis, aseptic meningitis, or partial facial paralysis result from involvement of the nervous system.
During pregnancy, chickenpox can lead to fetal infection and neonatal complications, but chronic infection or reactivation, or shingles, is not associated with fetal infection.
Herpes zoster Shingles is a painful entity on affected dermatomes without skin lesions.
Evaluation
Shingles is clinically diagnosed with burning pain, characteristic morphology and distribution. The herpes simplex virus can occasionally cause a rash in a pattern called herpes simplex zoster.
Tests for the varicella zoster virus may include:
Tsunk smear of vesicular fluid shows multinucleated giant cells. Less sensitive and specific than direct fluorescent antibody (DFA) or polymerase chain reaction (PCR).
Varicella-zoster virus-specific IgM antibodies in blood are detected during active infection with chickenpox or herpes zoster, but not when the virus is dormant.
If ocular lesions are present, vesicular fluid or corneal fluid can be tested directly using fluorescent antibodies.
PCR testing of follicular fluid, corneal lesions, or blood for ocular lesions or disseminated infections. Molecular biological tests (PCR tests) based on in vitro nucleic acid amplification are currently considered the most reliable.
Nested PCR tests are sensitive but prone to contamination leading to false positive results. Modern real-time PCR tests are quick, easy to perform, as sensitive as nested PCR, with less risk of contamination, and more sensitive than viral cultures.
The skin lesions associated with herpes zoster should be recognised from those associated with herpes simplex, dermatitis herpetiformis, impetigo, contact dermatitis, candidiasis, medication responses, and insect bites. Trigeminal neuralgia, renal colic, cholecystitis, biliary colic, and any tooth infection are not the same as prior discomfort without the emergence of shingles skin lesions.
Shingles tends to occur on only one side of the mouth, unlike other oral blisters. In the mouth, they first appear as vesicles that break up quickly, leaving ulcers that heal within 10 to 14 days. Precursor pain before the rash can be mistaken for toothache and lead to unnecessary dental work.
Treatment / administration
Antiviral therapy promotes lesion resolution, relieves acute pain, and helps prevent postherpetic neuralgia, especially in older patients. Antiviral drugs used to treat shingles include acyclovir 800 mg 5 times a day for 5 days, valacyclovir 1 g 3 times a day for 5 days, and famciclovir 500 mg 3 times a day for 7 days.
Topical antibiotic creams, such as mupirocin and soflamycin, help prevent secondary bacterial infections. Pain relievers help relieve pain. In some cases, severe pain may require opioid drugs. Topical lidocaine and nerve blocks can also reduce pain.
Postherpetic neuralgia is common in older patients, and topical capsaicin and emla cream can be used once the lesions have crusted over.
Differential diagnosis
- Cellulite.
- Chicken pox.
- Cnidarian poisoning.
- Contact stomatitis.
- Herpes simplex skin symptoms.
- Eczema.
- Erysipelas.
- Erysipelas.
- Folliculitis.
- Cowpox infection in humans.
- Irritant contact dermatitis.
- Insect bite.
- Striatal lichen.
- Mucosal candidiasis.
Improved health team outcomes
Shingles is a common infection in the elderly with significant morbidity. The disease cannot be cured, but vaccination can prevent most people with it. If eye lesions occur, patients should be referred to an ophthalmologist as soon as possible. Health care professionals, including family physicians, nurses, internists, and pharmacists, should educate patients about the benefits of vaccines.










