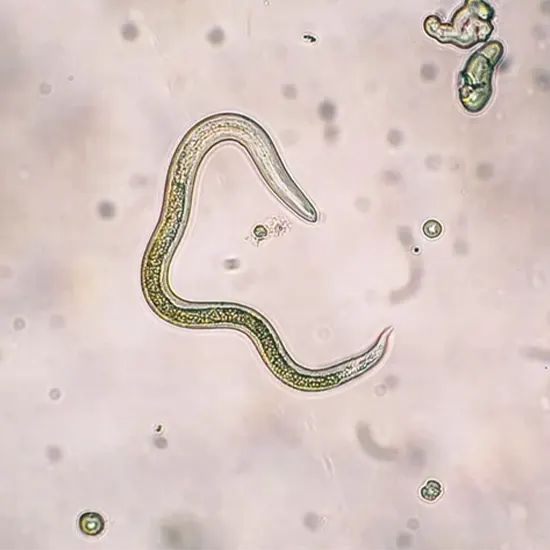
The larvae of Toxocara roundworms are the source of the parasitic ailment known as toxocariasis. The majority of the time, these worms affect dogs and cats, but they can also infect other surfaces by excreting parasite eggs...
What is Toxocariasis: Understanding the Parasitic Infection? The larvae of Toxocara roundworms are the source of the parasitic ailment known as toxocariasis. The majority of the time, these worms affect dogs and cats, but they can also infect other surfaces by excreting parasite eggs that can pollute the soil.
Humans can contract toxocariasis through coming into contact with the eggs on their skin or mucous membranes, inadvertently eating contaminated soil or dust, or both.
The larvae can move through different tissues and organs once they have entered the human body, causing a variety of symptoms depending on where they are. When the infection affects the eyes, it can lead to a condition called ocular larva , which, if ignored, can cause permanent visual loss.
Symptoms of Ocular Larva Migrans: How To Recognize Toxocariasis
Depending on where the larvae have moved in the body, toxocariasis can result in a variety of additional symptoms in addition to ocular larva . Toxocariasis symptoms frequently seen include:
- Fever
- Continent pain
- nausea and diarrhoea
- Fatigue
- Respiratory signs like coughing and wheezing.
Rarely, the infection may cause more serious side effects such organ damage or seizures.
It is crucial to remember that not everyone who has toxocariasis will exhibit symptoms, especially in cases of low-level exposure or when the larvae are still restricted to a single location of the body.
However, even those who are asymptomatic can still transmit the virus to others through their bodily fluids, such as their faeces.
You should consult a doctor for a diagnosis and treatment if you believe that you or someone you know may have been exposed to the Toxocara parasite. To ascertain the severity of the infection and the location of the larvae, this may entail a physical examination, blood tests, and other diagnostic imaging procedures. Most people with toxocariasis can recover totally and prevent long-term consequences with timely and adequate treatment.
Causes and Transmission: How Toxocara Larvae Spread?
Toxocara canis and Toxocara are parasitic roundworms that can be found in the intestines of dogs and cats, respectively. Toxocara larvae are the immature forms of these parasitic roundworms. Humans who are exposed to the larvae may get a disorder called toxocariasis, which can have severe health effects.
There are several ways that toxocara larvae might spread:
Consumption of contaminated soil : Toxocara eggs, which can contaminate soil, are shed in the faeces of diseased dogs and cats. The eggs can hatch in people's intestines when they swallow contaminated soil, and the larvae can then go to other areas of the body.
Consumption of tainted food or water : Toxocara eggs can taint food or water, especially in places with inadequate hygiene. The larvae can hatch in people's intestines and spread infection if they consume tainted food or water.
Direct contact with infected animals : People who come into direct contact with diseased animals, particularly puppies and kittens, can contract Toxocara larvae. The larvae can enter the human body through the skin, mouth, or nose after being shed in an animal's faeces, saliva, or other bodily fluids.
Transplacental transmission : In rare instances, a mother with toxocara infection may pass the infection to her unborn child through the placenta. The growing foetus may experience severe difficulties as a result of this.
Toxocara larvae must be prevented from spreading by using proper sanitation and hygiene practices. This entails completely cleaning your hands with soap and water after handling animals, avoiding contact with animal waste, and disposing of animal waste in an appropriate manner.
High-Risk Groups: Who is Most Susceptible to Toxocariasis?
Anyone who comes into contact with Toxocara larvae can become infected with toxocariasis, however some groups of people are thought to have a higher risk of infection or a greater propensity for developing a severe illness. Among these high-risk categories are the following:
Children: Children have a higher chance of contracting an illness because they are more likely to play in sandboxes or soil that has been contaminated with Toxocara eggs, and they may also be less likely to maintain proper hygiene practises such as frequent hand washing.
Owners of dogs or cats are more likely to contract the disease because these animals may pass Toxocara eggs in their waste, which can linger in the soil for years.
Immune system weaknesses : People who are receiving chemotherapy or who have HIV/AIDS have immune systems that are more vulnerable to severe types of toxocariasis.
Consumption of raw or undercooked meat by humans can enhance one's chance of contracting toxocariasis, especially if the meat comes from diseased animals.
Living in poverty : Communities with lower socioeconomic status are more likely to have poor sanitation and hygiene standards, as well as limited access to healthcare.
Exposure at work : Due to their frequent interaction with animals and polluted soil, certain occupations, such as veterinarians, animal handlers, and landscapers, may be more susceptible to contracting the toxocara infection.
These high-risk groups should take special care to prevent Toxocara infection, including maintaining pets that are adequately dewormed and avoiding contact with animal faeces.
Diagnosis of Toxocariasis
Imaging scans, laboratory tests, and clinical evaluations are frequently used to diagnose toxocariasis.
Clinical assessment : Typically, a healthcare professional will start by assessing the patient's symptoms, past health conditions, and potential exposure to Toxocara larvae. Numerous symptoms, such as fever, stomach ache, coughing, wheezing, and skin rashes, can be brought on by toxocariasis.
Serologic examinations : Blood tests can find antibodies to Toxocara larvae, which can support the toxocariasis diagnosis. The Western blot and the enzyme-linked immunosorbent assay (ELISA) are the two tests that are utilised the most frequently.
Imaging studies : To see any organ or tissue damage brought on by the larvae's migration, imaging tests like X-rays or ultrasound may be employed. For instance, an ophthalmologist may do a fundoscopic examination or employ imaging methods like optical coherence tomography (OCT) or ultrasonography in the case of ocular toxocariasis, which damages the eyes.
Rarely, a biopsy may be required to determine whether Toxocara larvae are present in the tissues in question.
It's crucial to remember that toxocariasis can be difficult to diagnose since the symptoms can resemble those of other illnesses and because serologic tests may result in false-negative results. Healthcare professionals must have a clinical suspicion of the illness based on the patient's medical history and symptoms, and they may need to consider additional diagnostic procedures to rule out other potential explanations of the patient's symptoms.
Treatment Options: Medications and Supportive Care for Toxocariasis
Medications to kill the Toxocara larvae and supportive care to manage any symptoms or problems are commonly used to treat toxocariasis.
Medication: Albendazole and mebendazole, both broad-spectrum anthelmintics that can kill the larvae, are the most frequently prescribed drugs for treating toxocariasis. Depending on how severe the illness is, the course of therapy may last from a few days to a few weeks.
Steroids: Corticosteroids may be used to treat severe inflammation brought on by migrating larvae in order to lessen swelling and irritation.
Treatment for symptoms: Other drugs or therapies might be suggested based on the symptoms and consequences that are present. Anti-inflammatory medications, for instance, may be used to treat fever or joint discomfort, whilst antihistamines may be used to treat skin rashes or allergic responses.
Treatment for the eyes: In situations of ocular toxocariasis, further therapies could be required to avoid long-term eye damage. These include laser photocoagulation, corticosteroid or anti-VEGF injections, and surgery to remove the damaged tissue.
Follow-up care: Toxocariasis patients must be continuously watched in order to manage any lingering symptoms or consequences and to make sure the infection has been successfully treated.
It's crucial to highlight that toxocariasis can be prevented from developing long-term consequences by receiving early diagnosis and treatment.
Prevention strategies for Toxocariasis
There are numerous easy steps people may take to lower their risk of contracting toxocariasis, which is a disease that is preventable:
Maintain good hygiene: After playing with pets, handling sand or mud, or working in areas where animal faeces may be present, wash your hands thoroughly with soap and water. Before washing your hands, avoid touching your face or mouth.
Maintain adequate deworming of pets: Deworming pets on a regular basis, particularly dogs and cats, can help cut down on the amount of Toxocara eggs they pass in their faeces. In order to determine the proper deworming schedule, speak with your veterinarian.
Avoid touching dirt or sand that may be contaminated with animal faeces, and dispose of animal waste promptly and correctly to prevent exposure to animal waste. Children shouldn't be allowed to play in regions with animal waste.
Cook meat thoroughly: Cook meat, particularly pig or beef, thoroughly to eradicate any potential Toxocara larvae.
Wear gloves and shoes: When gardening or working with soil, put on gloves and shoes. Avoid going barefoot in areas where there may be animal faeces.










