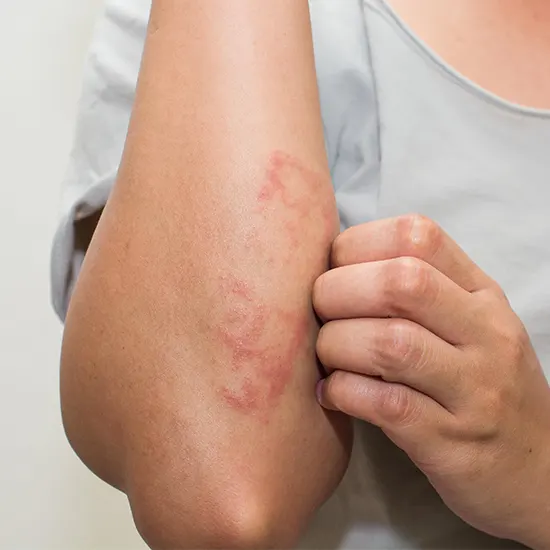
Eczema is a skin disease that results in red, dry, and itchy skin patches. Although it can appear anywhere on the body, the face, hands, feet, and folds of the skin are where it is most frequently located. Eczema...
Eczema
- Eczema is a skin disease that results in red, dry, and itchy skin patches.
- Although it can appear anywhere on the body, the face, hands, feet, and folds of the skin are where it is most frequently located.
- Eczema sufferers may be genetically predisposed to the condition, and aggravating factors like stress, allergies, and irritants can exacerbate it.
- eczema can cause severe itching and result in skin damage, making it a frustrating and unpleasant condition.
Statistics of Eczema incidence and Prevalence:
- Eczema incidence and prevalence can change based on elements like age, gender, location, and ethnicity.
- Around the world, up to 20% of toddlers and up to 3% of adults suffer from eczema, according to the World Allergy Organization. In the United States, it is believed that 10% of the population, or about 31.6 million people, suffer from eczema. Up to 20% of children in the U.S. experience eczema symptoms at some time in their lives, making it more prevalent in children. Adults can also be affected by the condition, which has a 1-3% prevalence rate in the general community.
- According to studies, some racial groups are more prone to eczema than others. For instance, those of African or Asian descent are more apt than those of European descent to experience eczema. Eczema also tends to occur in families, so there may be a genetic component to it.
Types of Eczema:
Eczema comes in various types, each with its own special set of signs and causes. The most typical kinds of eczema consist of:
- The most prevalent form of eczema, atopic dermatitis affects up to 20% of children and 3% of adults globally. It is characterized by skin that is dry, itching, and inflamed and that over time can become red, scaly, and thickened. Asthma and hay fever are two allergic diseases that frequently co-occur with atopic eczema.
- Touch dermatitis: It is a form of eczema that develops when an allergen or irritant, such as certain chemicals, metals, or plants, comes into touch with the skin. When exposed to an irritant or allergen, symptoms like redness, irritation, and blistering can appear within minutes to hours.
- Seborrheic dermatitis: The scalp, face, and other oily regions of the body are frequently affected by it. It is characterised by skin areas that are red, scaly, and sometimes flaky. Dandruff is frequently linked to seborrheic dermatitis, which can be brought on by stress, changing weather, and some medicines.
- Dyshidrotic eczema: This kind of eczema affects the sides of the extremities. It is characterized by tiny, excruciating, fluid-filled blisters that can itch. Stress, allergens, and exposure to specific metals can all cause dyshidrotic eczema, which is more prevalent in women.
- Nummular eczema: This form of eczema is characterized by coin-shaped, itchy, and painful red, scaly skin areas. It is more prevalent in men and is frequently brought on by dry skin, cold weather, and stress.
Why does this occur?
Here are a few potential dermatitis causes:
- Immune system dysfunction: Those who suffer from dermatitis have an overactive immune system that reacts to irritants or allergens by inflaming the skin. Redness, itching, and other signs may result from this.
- Environmental factors: Dry air, chilly temperatures, heat, sweating, and exposure to irritants like chemicals, detergents, and soaps can all cause or aggravate eczema symptoms.
- Allergies: Eczema frequently coexists with allergies, such as dietary allergens, environmental allergies, and sensitivity to specific substances or materials.
- Bacteria and viruses of kinds can also cause or aggravate the symptoms of eczema.
- Stress: For some individuals, emotional stress can make their eczema symptoms worse.
Genetics and Eczema:
- Numerous genes, including those involved in inflammation, immune system control, and skin barrier function, have been linked to dermatitis through research. These traits may have an impact on how the skin reacts to irritants, allergens, and microbes, which can cause eczema symptoms.
- For instance, eczema risk has been related to mutations in the filaggrin gene, which is essential for maintaining the function of the skin barrier. Other genes, including those related to the immune system, have also been linked to eczema, indicating a possible role for an abnormal immune reaction to environmental triggers.
- Even though heredity plays a significant role in eczema, it is not the only one. Other environmental variables that can cause or aggravate eczema symptoms include stress, the weather, and exposure to irritants and allergens.
Familial relationship of eczema:
- Even though having an eczema-prone family member increases the chance of developing the condition, it does not guarantee it. Eczema can form and get worse for a variety of reasons, including environmental triggers, stress, and lifestyle decisions.
- In order to lessen your risk of getting eczema or to avoid flare-ups, it is crucial to be aware of the symptoms and signs of the condition if you have a family history of it. You should also take precautions to manage any potential triggers.
- Some research history shows that eczema has been linked strongly to family history, and heredity probably plays a big part in how it develops. According to research, children who have one eczema-prone parent have a 50% chance of also getting the condition, while those who have two eczema-prone parents have an 80% chance.
Lifestyle and Eczema:
- Even though eczema can also be caused by living choices, genetics does play a part in its onset. Some living elements that can cause eczema or make it worse include:
- Irritants: Eczema can be brought on or made worse by exposure to irritants like soaps, detergents, perfumes, and specific textiles.
- Allergens: Certain foods, dust mites, pollen, and cat dander are just a few allergens that can cause eczema.
- Stress: Stress can impair immunity and cause or exacerbate dermatitis.
- Diet: For some people, eating things like dairy, eggs, wheat, and soya can start or aggravate eczema.
- Climate: Dry, cold conditions can make skin dry and itchy, which can start or aggravate eczema.
- activity: Some people's eczema can be brought on by vigorous activity that makes them perspire heavily.
- Scratching: Scratching causes skin harm and aggravates eczema.
Immunological factors responsible for Eczema:
Some of the immunological causes of dermatitis include the following:
- Skin barrier dysfunction: People who have eczema have a skin barrier function that is compromised, allowing irritants and allergens to enter the skin and resulting in an immune reaction.
- Eczema is linked to a type 2 immune reaction, which is characterized by cell activation and the production of cytokines like IL-4, IL-5, and IL-13. These cytokines encourage cutaneous itching and inflammation.
- Immunoglobulin E (IgE) antibodies: IgE antibodies, which are implicated in the allergic response, are more prevalent in eczema patients. IgE antibodies can attach to allergens and start an immune reaction that causes flare-ups of eczema.
- People who have eczema have a faulty innate immune system, which increases their susceptibility to infections and inflammation.
- Skin microbiome dysregulation: The microbes that inhabit the skin make up the skin microbiome. The skin microbiota is dysregulated in eczema patients, which can cause swelling and itching.
It is possible to create novel treatments for eczema, such as targeted biological drugs that can modify the immune response, by better understanding these immunological factors.
Symptoms that the patient encountered with eczema:
Eczema is a complicated condition that can be brought on by a mix of genetic and environmental factors, and everyone will experience it differently.
- Dry-itchy skin: The most typical signs of dermatitis include dry, itchy skin. Eczema sufferers frequently have difficult-to-alleviate continuous itching, which can damage their skin and increase their risk of infection. Eczema-affected skin can also develop raised bumps or blisters in areas and turn red and inflamed. The cheeks, neck, hands, and feet are just a few areas of the body where these patches can develop.
- Rash: An eczema rash can develop anywhere on the body, but the hands, feet, face, and neck are the most typical locations.
- Skin that is thickened and scaly: Eczema can occasionally cause the afflicted skin to become thickened and scaly.
- Skin cracks: The continuous scratching and itching associated with eczema can lead to painful skin cracks.
- Eczema can result in the development of tiny bumps or blisters on the skin.
- epidermis swelling: The affected epidermis may develop swelling and become sensitive to touch.
- Eczema can result in the development of tiny bumps or blisters on the skin.
- epidermis swelling: The affected epidermis may develop swelling and become sensitive to touch.
- Sensitivity to specific materials: People who have eczema may become sensitive to materials like soaps, detergents, and textiles.
- Sleep disturbances: It can be challenging to get a decent night's sleep when you have eczema due to the itching and discomfort it causes.
Diagnosis of Eczema:
- A healthcare professional, such as a dermatologist or allergist, will typically conduct a comprehensive physical examination and review your medical history in order to diagnose eczema. An outline of the testing procedure is provided below:
- Physical examination: The doctor will look for eczema symptoms like dryness, redness, itching, and inflammation on the afflicted skin.
- Medical history: The doctor will inquire about your symptoms, including when they first started and whether anything seems to be a cause. They might inquire if there is a history of allergies or dermatitis in the family.
- Skin patch test: A skin patch test may occasionally be used to ascertain whether you are allergic to a particular material, such as nickel or fragrances. This entails putting tiny amounts of various allergens on your skin and watching how they respond.
- Blood test: To rule out additional conditions that may manifest identical symptoms, such as a bacterial or fungal infection, a blood test may be prescribed.
- Skin biopsy: A skin biopsy may be done to confirm the diagnosis of eczema or to rule out other skin diseases in rare circumstances. To do this, a tiny sample of the affected skin must be taken and examined under a microscope.
The diagnosis of eczema is frequently based on a mix of physical exam findings, medical history, and ruling out other potential causes of the symptoms. It's essential to remember that there is no single test to identify eczema. It's critical to obtain medical advice from a healthcare provider if you think you may have eczema.
Home-Remedies for Eczema:
Eczema cannot be cured, but there are several home remedies that can help to control the condition's symptoms and offer relief. You can attempt the following natural remedies:
- Regular moisturizing is important for controlling the signs of eczema. At least twice daily, or more frequently, if necessary, moisturize the affected regions. To help keep hydration in, look for a thick, fragrance-free cream or ointment.
- Use mild, unscented products: Try to stay away from harsh cleansers, detergents, and other items that might irritate your skin. Look for hypoallergenic and items without fragrances.
- an oatmeal bath: To relieve itchy, irritated skin, add a cup of colloidal oats to a warm bath. The oatmeal will hydrate the epidermis and assist in reducing inflammation.
- Use coconut oil to reduce redness and itching: Coconut oil has anti-inflammatory properties that can aid. As required, apply a small quantity to the troubled areas.
- Use a humidifier: Dry air can make eczema symptoms worse, so keeping the air moist can help to avoid skin dryness.
- Aloe vera relieves itching and inflammation. Aloe vera gel has calming and cooling qualities. As required, apply a thin layer to the troubled regions.
- Try natural remedies: Tea tree oil, witch hazel, and apple cider vinegar are a few examples of natural remedies that some people use to treat their eczema problems. However, it's crucial to use prudence when using these treatments and to speak with a healthcare professional first.
- Home remedies can be useful for controlling the signs of eczema, but they should not be used in place of professional medical care.
Medical treatment for eczema:
The severity of the condition and the patient's particular symptoms will usually determine the course of medical treatment for eczema. Here are a few typical medicinal remedies for eczema:
- Topical steroids: Topical steroids are lotions or ointments used topically to treat skin conditions that cause inflammation. They are frequently employed to lessen irritation and soothe itching.
- Moisturisers: Managing the symptoms of eczema requires keeping the face well-hydrated. A medical professional might advise applying a thick, unscented cream or ointment to help retain hydration.
- Topical calcineurin inhibitors are non-steroidal lotions or ointments that are applied topically to treat itching and inflammation. When someone cannot tolerate or does not react to topical steroids, they are frequently prescribed.
- Systemic medications: A healthcare professional may recommend biologics, immunosuppressants, or oral steroids for the treatment of serious eczema. These drugs can be useful in treating symptoms because they help to lower inflammation throughout the body.
- Wet dressings: To soothe the epidermis and lessen inflammation, a damp dressing is applied to the affected region. People with severe eczema problems frequently use this treatment.
- Phototherapy: To lessen inflammation and itching, the epidermis is exposed to controlled levels of ultraviolet light. Individuals with mild to serious eczema symptoms frequently use this treatment.
The most effective eczema treatment strategy will depend on the unique symptoms and medical background of the patient, it is essential to note. For an accurate diagnosis and the best course of treatment, if you have eczema symptoms, it's crucial to seek medical guidance from a healthcare practitioner.
In conclusion, eczema is a widespread skin condition that can be uncomfortable and inflammatory, but there are numerous efficient treatments accessible to manage symptoms. There are many ways to relieve eczema symptoms and enhance the quality of life, ranging from mild household remedies to medical interventions like topical steroids and systemic drugs. Most people with eczema can have healthy, comfortable skin with appropriate management.
















