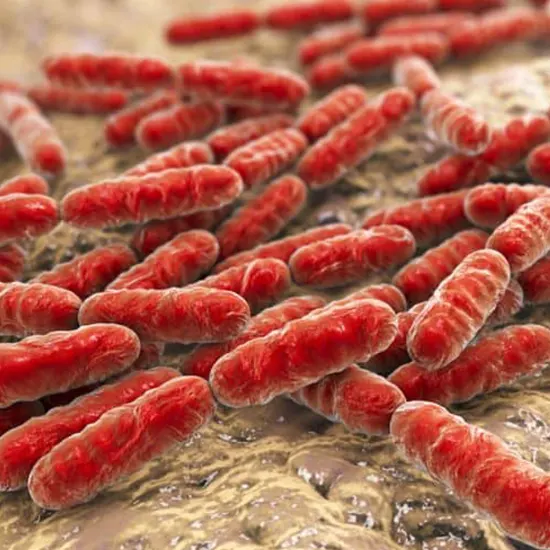
Small, aerobic, Gram-negative bacteria of the family Brucellaceae include the genus Brucella. This genus has several pathogenic species for both people and animals. Given their capacity to persist and reproduce inside the...
Small, aerobic, Gram-negative bacteria of the family Brucellaceae include the genus Brucella. This genus has several pathogenic species for both people and animals.
Given their capacity to persist and reproduce inside the cells of their hosts, Brucella species are categorized as facultative intracellular pathogens.
Humans can contract Brucella species by contact with sick animals, especially livestock like cattle, goats, and sheep, ingestion of contaminated food, inhalation of polluted aerosols, or ingestion of contaminated water.
Humans who are infected with Brucella can develop brucellosis, a febrile sickness characterized by symptoms including fever, chills, exhaustion, and joint pain.
Several Brucella species, including B. melitensis, B. abortus, B. suis, and B. canis, are important in CBC medicine. These species are widespread across the world and are known to transmit brucellosis to people.
The risk posed by Brucella species to the public's health is substantial, and brucellosis control and prevention efforts are continuing.
The many faces of Brucella: a closer look at Taxonomy
Each species of the genus Brucella of bacteria is linked to a specific host animal and is capable of causing brucellosis, a zoonotic illness that can infect both people and animals.
A list of Brucella species is provided below:
Brucella abortus
Brucella abortus is a species that is predominantly connected to cattle and may induce both human undulant fever and abortion in cows.
Brucella melitensis
Brucella melitensis is a species that is mostly connected to goats and sheep and may infect both animals and people with brucellosis.
Brucella suis
Brucella suis is a species that is mostly linked to pigs, while it can also infect people and other animals.
Brucella canis
Brucella canis is a species that is mostly linked to dogs and that can lead to infertility as well as other reproductive issues in dogs.
Brucella suis
Sick pork products or contact with sick animals can spread Brucella suis, which infects pigs and causes brucellosis, to people.
Brucella neotomae
In the southwest of the United States, desert woodrats are home to Brucella neotomae.
Brucella pinnipedialis
Found in seals.
Brucella ceti
Found in cetaceans (whales, dolphins, and porpoises),
Brucella microti
Found in mice and voles.
Brucella inopinata
Recently found in a breast implant infection.
Brucella papionis
Baboons are known to carry Brucella papionis.
Brucella vulpis
Among red foxes, Brucella vulpis is prevalent.
Size doesn't matter: exploring the unique morphology of Brucella species.
Small, Gram-negative, non-motile, non-spore-forming coccobacilli called Brucella species generally have dimensions of 0.5-0.7 mm in width and 0.6-1.5 mm in length.
The following are some key characteristics of Brucella morphology:
Small size
Brucella cells are much smaller than those of most other bacteria and can hardly be seen with the naked eye.
Shape
Coccobacilli, which have a rounded or oval form that is in between a coccus' (spherical) and a bacillus' (rod-shaped), are what Brucella cells are made of.
Lack of flagella
Brucella cells lack flagella and other features that allow for movement, making them nonmotile.
Absence of capsule
Brucella cells do not create a capsule, a barrier that certain bacteria utilize to evade the immune systems of their hosts.
Intracellular lifestyle
Brucella cells have an intracellular lifestyle and may survive and reproduce inside host cells as facultative intracellular pathogens.
High infectious dose
Brucella cells are extremely contagious, and just a few of them are enough to harm an unprepared host.
Slow growth
Brucella cells grow slowly and must be grown in certain conditions and mediums.
Size and shape
Variability:Brucella cells can fluctuate in size and form according to the development circumstances, making it challenging to identify them just based on morphology.
Overall, Brucella cells are microscopic and live an intracellular existence, making it challenging to observe and study them, but LFT their capacity to infect people and other animals makes it crucial to comprehend their shape and biology.
The range of clinical presentations in Brucella infections
Brucellosis, also known as Malta fever, undulant fever, or Mediterranean fever, is a zoonotic illness that can be brought on by the species of Gram-negative bacteria known as Brucella.
Brucella bacteria infect a broad variety of mammals, including domestic and wild animals, and can be passed from one animal to another or Echocardiography through contaminated animal products, including unpasteurized milk and cheese, to people through contact.
The symptoms of brucellosis in people might include fever, chills, headache, soreness in the muscles and joints, weariness, and weight loss. The condition may progress to chronicity and bring on side effects including endocarditis, rheumatoid arthritis, and neurological conditions.
In animals, brucellosis can result in generalized illness with fever, anorexia, and weight loss as well as reproductive issues such as abortion, stillbirth, and infertility.
The four Brucella species that affect people most frequently are B. abortus, B. melitensis, B. suis, and B. canis. Each species has a distinct spectrum of hosts and is connected to various routes of CT Head transmission and clinical manifestations. These species can transmit infections that vary from having minor flu-like symptoms to serious, chronic illnesses.
Globally speaking, brucellosis is a serious public health issue, especially in areas with subpar animal husbandry methods and Urine Routine subpar sanitation. Animal immunization programs and avoiding high-risk food items are two preventative options for the illness, which can be challenging to identify and treat.
Detecting the invisible: the laboratory techniques used to diagnose Brucella infections
Due to the vague symptoms of brucellosis, a combination of many laboratory techniques is typically necessary for a conclusive diagnosis.
Some techniques used often to identify Brucella infections are listed below:
Serology
Serological tests identify the existence of anti-Brucella antibodies in the blood of those with the disease. The Rose Bengal test, the most widely used serological test, is quick and affordable but less accurate than other tests like the serum agglutination test and the enzyme-linked immunosorbent assay (ELISA).
Culture
Using a specialized medium and favorable growth conditions, Brucella bacteria may be isolated from clinical samples such as blood, bone marrow, and bodily fluids. Due to the high infectiousness of the Urine Culture organism, culture is the gold standard for diagnosing brucellosis but is time-consuming and necessitates biosafety level 3 facilities.
Polymerase chain reaction (PCR)
PCR has high sensitivity and specificity for detecting Brucella DNA in clinical samples. But PCR needs specialized tools and knowledge, and it might be hampered by inhibitors in the material.
Imaging tests
Imaging tests including X-rays, computed tomography (CT), and magnetic resonance imaging (MRI) may help spot brucellosis-related complications such as osteomyelitis, abscesses, and meningitis.
Combating brucella infections with a comprehensive treatment plan
Depending on the severity of the infection and the Brucella species involved, brucellosis can be treated with a combination of antibiotics for several weeks to months.
Some of the typical antibiotics for treating Brucella infections are listed below:
Doxycycline
For the treatment of brucellosis, this antibiotic is frequently used with rifampin. It has high penetration into bone tissue and is well tolerated.
Rifampin
To treat brucellosis, this antibiotic is frequently used with doxycycline or another drug, such as streptomycin. It can assist remove terms from the bone marrow and has strong intracellular penetration.
Streptomycin
For the treatment of brucellosis, this antibiotic is frequently used with doxycycline or rifampin. It can help eliminate microorganisms and has strong tissue penetration.
Gentamicin
For the treatment of brucellosis, this antibiotic is also used in conjunction with other antibiotics. It may be administered intravenously and has strong anti-Brucella bacterial action.
Trimethoprim-sulfamethoxazole
This antibiotic combination, particularly in situations of recurrence, can be used to treat mild to moderate cases of brucellosis.
For the treatment of brucellosis symptoms, supportive care such as pain management, fever control, and hydration may be required in addition to medications.
To drain abscesses or remove contaminated tissue, surgery may occasionally be necessary.
To avoid complications and lower the chance of recurrence, early diagnosis, and treatment are essential.
Don't let brucellosis get under your skin: prevent Brucella infection.










