Tetanus is a dangerous bacterial illness that damages the nervous system and is sometimes referred to as lockjaw. The bacteria Clostridium tetani, which may be found in dust, dirt, and animal feces, is what causes the illness.
Tetanus is a dangerous bacterial illness that damages the nervous system and is sometimes referred to as lockjaw. The bacteria Clostridium tetani, which may be found in dust, dirt, and animal feces, is what causes the illness. Through a cut or wound, the bacteria enter the body and then release a toxin that affects the neurons that regulate muscular action.
This can result in muscular rigidity, spasms, and stiffness, especially in the jaw and neck muscles, which can make it difficult to breathe and swallow. If untreated, tetanus can develop life-threatening problems in the chest, abdomen, and limbs, among other areas of the body. Tetanus can be avoided by immunization, and if an infection is detected, urgent medical attention is crucial.
Tetanus through the Ages: From battlefield wounds to routine vaccinations
Since ancient times, tetanus, often known as lockjaw, has been recognized as a medical problem. The Greek physician Hippocrates originally documented the signs and symptoms of tetanus in the fifth century BCE. The word "tetanus" derives from the Greek word "tetanus," which means "stiff," and refers to the disease's distinctive muscular stiffness.
The bacteria Clostridium tetani were discovered to be the source of tetanus by German doctor Arthur Nicolaier in the 19th century. Shortly after, the French doctor Pierre Paul Émile Roux used heat-neutralized tetanus toxin to create a vaccination to prevent tetanus. This was one of the earliest examples of a toxoid vaccine, which induces immunity by using a modified form of the toxin that is no longer harmful.
In the early 20th century, tetanus vaccination became widely available, and the incidence of tetanus declined dramatically in developed countries. Today, tetanus is relatively rare in countries with high vaccination rates, but it remains a significant public health concern in developing countries where access to vaccines and medical care is limited.
The bacterial culprit behind tetanus- Clostridium tetani
The bacteria Clostridium tetani cause lockjaw.
A wound, cut, or puncture might allow the germs to enter the body, especially if it is deep, filthy, or polluted with soil or animal feces.
Injuries that injure the skin and reveal the underlying tissues, such as burns, frostbite, or any other sort of injury, can also allow germs to enter the body.
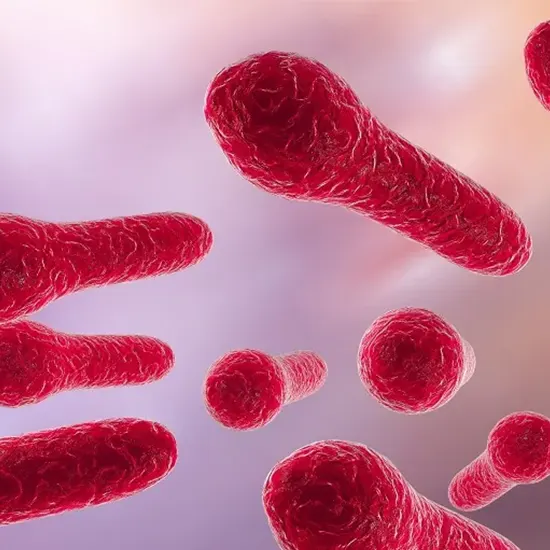
A rod-shaped bacterium, or one with a cylindrical form and rounded ends, is Clostridium tetani.
With a diameter of around 0.5-0.8 micrometers and a length of roughly 2-4 micrometers, the bacterium is comparatively big.
Gram-positive bacteria, such as Clostridium tetani, have thick layers of peptidoglycan in their cell walls that help them hold onto the crystal violet stain during the gram-staining process.
Because the bacteria is anaerobic, it thrives in conditions with little or no oxygen.
The peritrichous flagella that cover the cell surface are what allow the motile Clostridium tetani to move.
Endospores are in structures that the bacteria format is dormant, robust, and extremely resistant to extreme environmental conditions including heat, radiation, and chemicals. The drumstick-like look of Clostridium tetani is due to the oval-shaped spores that are present at the end of the bacterial cell.
Tetanospasmin, a strong neurotoxin that the bacteria can produce and is what causes tetanus symptoms.
From bacteria to toxin: The journey of tetanus infection
The toxin-producing bacteria Clostridium tetani are responsible for tetanus.
A wound, cut, or puncture might allow the bacteria to enter the body, especially if it is deep, filthy, or polluted with soil or animal feces.
When a bacteria enters the body, it multiplies and begins to create tetanospasmin, a strong neurotoxin that harms the neurological system.
Tetanospasmin enters the central nervous system where it disrupts inhibitory neurons' ability to carry out their regular functions, which regulate muscular relaxation.
This causes muscular rigidity, spasms, and stiffness, especially in the jaw and neck muscles, which can make it difficult to breathe and swallow.
Tetanospasmin can cause muscular contractions and spasms in different areas of the body as the illness worsens, including the chest, abdomen, and limbs.
Tetanus can cause life-threatening consequences including respiratory failure, pneumonia, and cardiac arrest in severe instances.
The quantity of toxin generated, the length of exposure, and the patient's immunological response are some of the variables that affect how severe the disease will be.
Tetanus does not provide long-lasting protection, and if the germ is introduced again, a person may contract it once more. Tetanus may be prevented most successfully with vaccination.
From stiffness to spasms: Understanding the symptoms of tetanus
Tetanus typically takes 3 to 21 days to incubate, with an average of 8 days.
Muscle stiffness and spasms in the jaw and neck are frequently the first signs of tetanus, which can make it difficult to open the mouth or swallow.
The stiffness and spasms, which can be unpleasant, might affect different bodily areas, such as the chest, abdomen, and limbs.
Fever, perspiration, increased blood pressure, and an accelerated heartbeat are some other signs of tetanus.
Tetanus can induce rigidity and stiffness in the muscles in severe instances, making it difficult to move or breathe. This may result in potentially fatal consequences such as respiratory failure, pneumonia, and cardiac arrest.
Tetanus can induce highly painful and violent spasms that can be brought on by external stimuli like touch, light, or noise.
Tetanus can also disrupt the autonomic nervous system, resulting in symptoms including excessive perspiration, blood pressure swings, and a fast heartbeat.
Patients may have trouble breathing as the condition worsens and may need mechanical ventilation to sustain their respiratory function.
Up to 30% of instances of tetanus can result in death, especially in people who are unvaccinated and who get insufficient or delayed care.
Tetanus: Diagnosing the disease for effective treatment
Tetanus is normally diagnosed using a combination of laboratory testing, physical examination, and medical history. Here are some important details about tetanus diagnosis:
Patient History
The physician will inquire about the patient's recent history of wounds or injuries, immunization status, and symptoms since the medical history of the patient is crucial.
Symptoms
Muscle rigidity, spasms, and stiffness will be specifically looked for during the physical examination, with the jaw and neck muscles receiving the most attention. Additionally, the doctor may look for symptoms of autonomic nervous system dysfunction, such as sweating, an accelerated heartbeat, and blood pressure swings.
Blood Tests
Blood tests to check for tetanus antibodies or to evaluate kidney and liver function may be used as laboratory testing to assist confirm the diagnosis of tetanus.
Cultures
It is also possible to do a culture of the wound site or blood to isolate the bacteria Clostridium tetani, albeit this is not always feasible.
Electromyography (EMG)
To evaluate nerve function and find anomalies, further procedures like electromyography (EMG) or nerve conduction investigations may be carried out.
Tetanus is largely diagnosed based on clinical manifestation, and laboratory testing is often illustrative rather than conclusive. It is crucial to remember that a negative laboratory test result does not always rule out the potential of tetanus; instead, the diagnosis should be based on the patient's specific signs and symptoms.
Even if the diagnosis has not been established, therapy should start right once in situations with suspected tetanus.
Tetanus: Treating the disease for a better outcome
Tetanus is normally treated with a mix of supportive care, wound care, tetanus antitoxin therapy, and antibiotics. Here are some essential details about tetanus treatment:
Supportive Care
Measures to control muscular spasms such as bed rest, a calm setting, and sedatives or muscle relaxants are examples of supportive care. In extreme situations, mechanical ventilation and respiratory assistance may also be necessary.
Wound Debridement
To treat a wound, it must be cleaned, debrided of any contaminated tissue, and given medicines to stop the spread of infection.
Anti-toxin
Tetanospasmin toxin, which is generated by Clostridium tetani, can be neutralized by the preparation of antibodies known as tetanus antitoxin. When tetanus is suspected, it should be treated as quickly as possible, ideally within 24 hours after the beginning of symptoms.
Antibiotics
To stop the growth and spread of the Clostridium tetani bacterium, antibiotics are given. For this reason, penicillin or metronidazole are frequently utilized.
Immunoglobulin Therapy
In addition to supportive care, wound care, tetanus antitoxin, and antibiotics, other therapies may be employed. These include immunoglobulin therapy, which can offer momentary immunity against tetanus, and magnesium sulfate, which can assist manage muscular spasms.
It is essential to remember that tetanus treatment can be difficult and may call for extended hospitalization and special care. Mortality rates can be significant in serious instances, especially in those who have not had vaccinations or whose medical care has been delayed or is insufficient.
Tetanus can be prevented most effectively by vaccination, hence it should be a part of everyone's normal immunization plan.
Tetanus : The battle we can win through awareness and action









