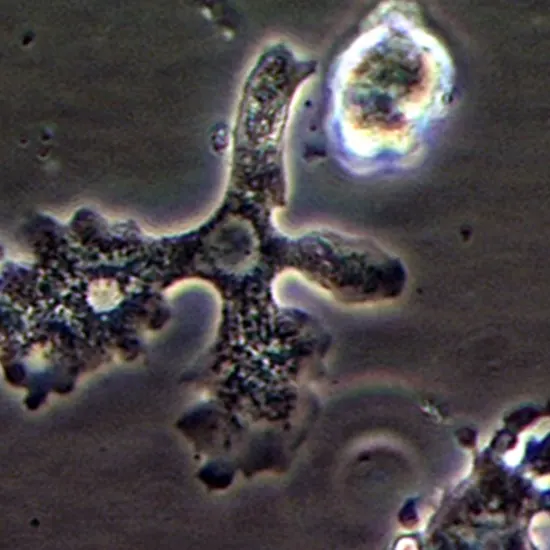
Single-celled microorganisms known as free-living amoebae can be found in soil, water, and other habitats that are present in nature. Although the majority of free-living amoeba species are benign, some of them can infect people.
Single-celled microorganisms known as free-living amoebae can be found in soil, water, and other habitats that are present in nature. Although the majority of free-living amoeba species are benign, some of them can infect people. The amoeba Naegleria fowleri is one of the most well-known and dangerous kinds of free-living amoebic infections and can cause primary amebic meningoencephalitis (PAM), an uncommon but frequently deadly brain infection.
Warm freshwater environments including lakes, rivers, and hot springs are where N. fowleri is typically found. Infection happens when the amoeba-containing water enters the body by the nose, usually during diving or swimming. The amoeba can then ascend the olfactory nerve to the brain, where it causes inflammation and brain tissue loss.
Avoiding activities in warm waters that might cause water to enter the nose, such as diving, leaping, and water skiing, will help prevent free-living amoebic infections. It is advised to hold your nostrils shut or wear nasal plugs when engaging in water sports. Additionally, as contact lens keratitis risk is increased by non-sterile water exposure, it's crucial to avoid using non-sterile water on your contact lenses.
Tracing the origins of free-living amoebic infections through history
Primary amebic meningoencephalitis (PAM), a rare but fatal infection brought on by the free-living amoeba Naegleria fowleri, was first recognized in a patient in 1965. A little child from Australia who had been swimming in a warm freshwater lake at the time of the incident passed and died quickly after exhibiting indications of brain infection.
Since then, hundreds of PAM cases have been recorded around the globe, with the United States and Australia MRI Brain having the greatest incidence rates. The majority of instances in the United States take place in the southern states, particularly in the summer when the water is warmer.
Another kind of free-living amoebic illness called Acanthamoeba keratitis was first documented in 1973.
Since the amoeba can become stuck beneath the lens and spread an infection to the eye, contact lens usage is often linked to this Blood Glucose infection. Acanthamoeba keratitis is an uncommon but severe illness that can impair eyesight and calls for immediate medical attention.
Overall, free-living amoebic infections continue to be an uncommon but important public health issue, especially in warm freshwater regions and among people with compromised immune systems or contact lens wearers.
Know the culprits: causes and sources of free-living amoebic infections
There are numerous different kinds of free-living amoebae that can infect people. Among the most frequent agents responsible for free-living amoebic infections are:
Naegleria fowleri
Primary amebic meningoencephalitis (PAM), an uncommon but sometimes deadly brain infection, is caused by Naegleria fowleri. In warm freshwater areas like lakes and rivers, N. fowleri is generally present and can enter the body by the nose when diving or swimming.
Acanthamoeba species
Acanthamoeba species are frequently responsible for Acanthamoeba keratitis, a dangerous eye illness that is frequently linked to the use of contact lenses. Acanthamoeba can also cause skin infections and, in rare instances, granulomatous amoebic encephalitis (GAE), a systemic illness.
Sappinia diploidea
Sappinia diploidea is a newly discovered amoeba that has been linked to a small number of infections in people. S. diploidea inhabits watery settings and can go inside people through the mouth or nose.
Generally speaking, free-living amoebic infections are uncommon but devastating illnesses that can have a major impact on morbidity and death. Prevention strategies are essential for lowering the risk of illness, including avoiding contaminated water exposure and maintaining excellent hygiene.
The remarkable morphology of Naegleria fowleri: a closer look
Primary amebic meningoencephalitis (PAM), an uncommon but sometimes deadly brain illness, is brought on by the free-living amoeba Naegleria fowleri. The following standout characteristics of Naegleria fowleri's morphology:
Size
Naegleria fowleri is a very big amoeba, with a normal diameter of between 8 and 15 micrometers.
Form
Although N. fowleri can take on a variety of shapes, it is normally ameboid, which means that it can modify its form and move by extending and retracting pseudopodia (cell membrane projections).
Single, sizable nucleus
The nucleus of N. fowleri is usually found close to the center of the cell.
Cysts
N. fowleri may produce latent, resilient structures called cysts in response to unfavorable environmental circumstances, which aid the amoeba in surviving in severe settings. These cysts are usually spherical and range in size from 7 to 10 micrometers.
Motility
Flagella are whip-like structures that aid in motility, however, N. fowleri lacks them in contrast to certain other species of amoebae.
Shape
Naegleria fowleri has a general shape that is comparable to other free-living amoebae, but it has special traits that enable it to live in warm freshwater habitats and cause life-threatening infections in people.
Beyond brain-eating: the diverse types of free-living amoebic infections
Humans are susceptible to a variety of free-living amoebic diseases, including:
Primary amebic meningoencephalitis (PAM)
Naegleria fowleri is the cause of the uncommon but frequently deadly infection known as primary amebic meningoencephalitis (PAM). The amoeba enters the body through the nose, moves to the brain, and damages brain tissue by inflaming it.
Acanthamoeba keratitis
An infection of the cornea brought on by the amoeba Acanthamoeba is known as acanthamoeba keratitis. It can result in significant eye discomfort, redness, and vision loss and is frequently linked to the usage of contact lenses.
Amoebic encephalitis (GAE)
The rare but dangerous condition known as granulomatous amoebic encephalitis (GAE) is brought on by several distinct free-living amoebae, such as Acanthamoeba and Balamuthia mandrillaris. It often affects those with low immune systems and can harm the brain by inflaming it.
Free-living amoebic infections are generally uncommon but dangerous illnesses that can have a considerable impact on morbidity and death. The risk of infection can be decreased via the use of preventative measures such as proper hygiene practices and avoiding contact with polluted water.
The hunt for amoebae : approaches to the diagnosis of free-living amoebic infections
Due to the rarity of these illnesses and the vague symptoms they might produce, diagnosing free-living amoebic infections can be difficult. However, identifying these infections may be done using some diagnostic techniques:
Clinical assessment
Finding potential instances of free-living amoebic infections requires a comprehensive clinical assessment. Symptoms may include fever, headache, nausea, vomiting, seizures, and neurological impairments, depending on the infection type.
Laboratory testing
Laboratory tests can be performed to determine if samples like cerebrospinal fluid (CSF), eye swabs, or skin biopsies contain free-living amoebae. These examinations could make use of microscopy, culture, or PCR-based techniques.
History of travel
Travel to regions with a higher prevalence of free-living amoebic illnesses can assist support a diagnosis.
Healthcare professionals must retain a high index of suspicion in patients with similar symptoms, especially those who have a history of contact with polluted water sources. Free-living amoebic infections are uncommon and sometimes challenging to detect.
Fighting back against free-living amoebic infections: current treatment options
Due to their rarity and the absence of available therapeutic medications, free-living amoebic infections can be difficult to treat. To lower morbidity and mortality, treatment frequently focuses on Giemsa Stain for Free Living Amoebae symptom management and supportive care. Depending on the kind of illness and the severity of the symptoms, different therapies may be necessary.
Primary amebic meningoencephalitis (PAM): Naegleria fowleri causes PAM, which frequently results in death and for which there is no particular cure. An intensive care unit environment may include supportive treatment, such as managing seizures and brain edema.
Acanthamoeba keratitis
Antimicrobial drugs like chlorhexidine and propamidine are frequently used to treat this condition, along with supportive treatment for discomfort and inflammation.
Cutaneous amoebiasis
Treatment of cutaneous amoebiasis typically involves the use of antimicrobial agents such as chlorhexidine or pentamidine, along with wound care and supportive care for pain.
In addition to medical treatment, prevention measures are essential for reducing the risk of free-living amoebic infections. These may include avoiding exposure to contaminated water sources, practicing good hygiene, and using appropriate protective measures during water-related activities.
Don't give up the fight: Hope and determination in the face of free-living amoebic infections










