Uterine sarcomas can develop in different types of tissue, including the myometrium (the muscular layer of the uterus), the endometrium (the lining of the uterus), or the connective tissue that supports the uterus. There are...
Your fight is our fight, All you need to know about uterine sarcoma.
An outline
The muscles or supporting tissues of the uterus can develop into uterine sarcoma, a rare form of cancer which is called Uterine Sarcoma.
It is different from the more common type of uterine cancer called endometrial cancer, which originates in the lining of the uterus.
Uterine sarcomas can develop in different types of tissue, including the myometrium (the muscular layer of the uterus), the endometrium (the lining of the uterus), or the connective tissue that supports the uterus. There are several different subtypes of uterine sarcoma.
Uterine sarcomas are relatively rare, accounting for only about 3% to 7% of all uterine cancers. They tend to occur more often in women over the age of 50, and the risk factors for uterine sarcoma are not well understood.
Uterine sarcoma can be difficult to diagnose, as the symptoms are often similar to those of other gynecological conditions, such as fibroids or endometriosis.
Treatment for uterine sarcoma may involve surgery to remove the uterus (hysterectomy) or other affected tissues, as well as radiation therapy and chemotherapy.
This article will reflect upon the various causes, symptoms, and treatment options for uterine sarcomas.
Know the Prevalence
According to the American Cancer Society, uterine sarcomas make up less than 5% of all uterine cancers, with approximately 4 out of 100 women with uterine cancer having uterine sarcoma. Uterine sarcoma is more common in women who have gone through menopause, and the risk increases with age.
Understanding the causes and associated risk factors of uterine sarcomas
The exact cause of uterine sarcoma is not well understood, but certain risk factors have been identified that may increase a person's chances of developing this rare type of cancer. Here are some of the possible causes and risk factors:
- Genetic mutations: In some cases, genetic mutations may be responsible for the development of uterine sarcoma.
- Radiation exposure: Women who have received pelvic radiation therapy for other types of cancer, such as ovarian cancer, may be at a higher risk of developing uterine sarcoma. Exposure to high doses of radiation during accidents, such as the Chernobyl disaster, can also increase the risk of developing uterine sarcoma.
- Hormonal factors: Women who have taken estrogen alone (without progesterone) for a long period may have an increased risk of uterine sarcoma. This is because estrogen can stimulate the growth of uterine tissue, which can lead to the development of cancer.
- Age and menopause: Uterine sarcoma is more common in women who have gone through menopause. With age, there is a higher chance of getting this cancer.
- Family history: Women with a family history of uterine sarcoma or certain types of cancer, such as breast or ovarian cancer may increase the risk of developing this type of cancer.
- Obesity: Being overweight or obese can increase your risk of developing uterine sarcoma.
History of uterine cancer
Women with a history of uterine cancer may be at elevated development of uterine sarcoma.
- Uses of Tamoxifen: Tamoxifen is a drug used to treat and prevent breast cancer. but it is linked to an increased risk of developing uterine sarcoma.
- Exposure to certain chemicals: Exposure to certain chemicals such as phenoxy methylphenoxyacetic acid is associated with an increased risk of developing uterine sarcoma.
- Medical history: Women with a history of pelvic inflammatory disease, endometriosis, or certain types of medical conditions like Benign uterine tumors may increase the risk of developing uterine sarcoma.
It's important to note that these risk factors do not guarantee that a person will develop uterine sarcoma but People who develop uterine sarcoma have no known risk factors.
Know the signs, and beat uterine sarcoma
Several risk factors have been found that increase the chance of developing this unusual type of cancer.
Here are some possible causes and risk factors:
- Abnormal vaginal bleeding: One of the most common symptoms of uterine sarcoma is abnormal vaginal bleeding. Bleeding between periods, heavy periods, postmenopausal bleeding, etc.
- Pelvic pain or pressure: Women with uterine sarcoma may experience pelvic pain or pressure that is not related to their menstrual cycle.
- Abdominal swelling: As the tumor grows, it may cause abdominal swelling or bloating.
- The feeling of fullness or heaviness in the abdomen: Women with uterine sarcoma may feel a sense of fullness or heaviness in their abdomen, even if they have not eaten much.
- Pain during sex: Some women with uterine sarcoma may experience pain during sexual intercourse.
- Anemia: Uterine sarcoma can cause anemia, which may lead to fatigue, weakness, and shortness of breath.
- Weight loss: In advanced cases, uterine sarcoma can cause unintentional weight loss.
- Difficulty urinating or defecating: Uterine sarcoma can cause pressure on the bladder or rectum, leading to difficulty urinating or defecating.
- Swelling in the legs: In rare cases, uterine sarcoma can cause blockage of the lymphatic vessels, leading to swelling in the legs.
- Pain in the legs: In advanced cases, uterine sarcoma may spread to the surrounding tissues, such as the bones and muscles of the legs, causing pain and discomfort.
- Constipation or diarrhea: Uterine sarcoma can cause changes in bowel habits, such as constipation or diarrhea.
- Nausea and vomiting: In advanced cases, uterine sarcoma can cause nausea and vomiting due to the tumor pressing against the digestive organs.
It's important to keep in mind that these symptoms can also be caused by other conditions, and having any of them does not necessarily mean that a person has uterine sarcoma To find out the underlying reason and get the right care, you should consult your doctor if you are having any of these symptoms, especially if they are persistent or getting worse over time.
From leiomyosarcoma to undifferentiated sarcoma: Know the complexities of uterine sarcoma
There are several types of uterine sarcoma, each of which is classified based on the type of cell that cancer starts in. The four main types of uterine sarcoma are:
- Leiomyosarcoma: This is the most common type of uterine sarcoma, accounting for about 50-60% of cases. Leiomyosarcoma begins in the smooth muscle cells of the uterus, which are responsible for the uterus's contractions during labor and delivery.
- Endometrial stromal sarcoma: This type of uterine sarcoma starts in the connective tissue cells that support the endometrium, which is the inner lining of the uterus. Endometrial stromal sarcoma accounts for about 15-20% of uterine sarcoma cases.
- Adenosarcoma: This rare type of uterine sarcoma starts in the glandular cells of the uterus and can spread to other parts of the body. Adenosarcoma accounts for about 5-10% of uterine sarcoma cases.
- Undifferentiated sarcoma: This is a rare and aggressive type of uterine sarcoma that starts in the mesenchymal cells, which are the cells that can develop into different types of tissues in the body. Undifferentiated sarcoma accounts for about 10-15% of uterine sarcoma cases.
It's important to note that uterine sarcoma is rare, and these types of uterine sarcoma are also rare. The type of uterine sarcoma a person has can affect their treatment options and prognosis.
Uterine sarcoma: Early detection saves lives
Uterine sarcoma is a rare but aggressive form of cancer that occurs in the muscles or connective tissues of the uterus. Diagnostic tests for uterine sarcoma may include clinical, laboratory, and radiographic tests. Here are some of the most common diagnostic tests for uterine sarcoma:
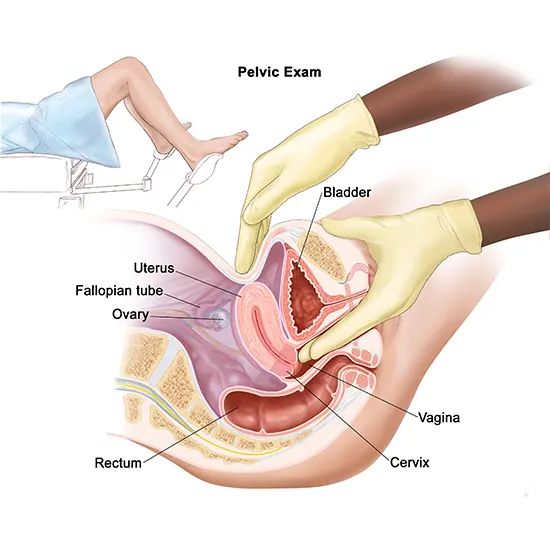
Pelvic Exam: The first step in diagnosing uterine sarcoma is a pelvic exam, which involves the doctor examining the uterus, vagina, ovaries, bladder, and rectum for any abnormalities.
Transvaginal ultrasound: A transvaginal ultrasound produces pictures of the uterus, ovaries, and other pelvic organs using high-frequency sound waves. Any tumors or other abnormalities in the uterus can be found with the use of this test.
Magnetic resonance imaging (MRI): Using strong magnets and radio waves, magnetic resonance imaging (MRI) produces precise pictures of the body. Any malignancies in the uterus and the surrounding tissues can be better located and sized with this method.
Computed Tomography (CT) Scan: A CT scan produces in-depth pictures of the body using X-rays and a computer. Any cancers in the uterus and the surrounding regions can be found with this test.
Biopsy: A biopsy is a procedure in which a tiny sample of uterine tissue is removed and examined under a microscope to check for the presence of cancer cells.
Blood testing: Blood tests can help identify any irregularities in blood cell counts, liver function, or kidney function that may be signs of uterine sarcoma.
Dilation and Curettage (D&C): During a D&C, the cervix is dilated, and uterine tissue is removed for microscopic analysis. This test can assist in identifying uterine sarcoma and assess cancer's stage.
Positron Emission Tomography (PET) Scan: A PET scan makes use of a radioactive tracer to identify parts of the body that are metabolically active or expanding rapidly, This may indicate the presence of cancer cells.
Abdominal and Pelvic CT with Contrast: This type of CT scan uses a contrast dye to help identify areas of the body with increased blood flow, which can indicate the presence of cancer cells.
CA-125 Blood Test: The level of CA-125 is determined by this blood test which is a protein that can be elevated in the presence of certain cancers, including uterine sarcoma. However, this test is not specific for uterine sarcoma. also increases under other conditions
Endometrial Sampling: This involves sampling the lining of the uterus to look for abnormal cells or cancer.
It's significant to remember that not every person with suspected uterine sarcoma may require all of these tests.
A healthcare practitioner will choose the precise diagnostic procedures based on the patient's symptoms, medical history, and other variables.
Comprehensive treatment care for women battling uterine sarcoma
The kind and stage of the malignancy, as well as the patient's health and other circumstances, affect the treatment choices for uterine sarcoma.
Medicines:
a) Chemotherapy: Chemotherapy is a systemic treatment that uses drugs to kill cancer cells throughout the body. It can be used as the main form of treatment for advanced uterine sarcoma or administered before or after surgery or radiation therapy. Common chemotherapy drugs used to treat uterine sarcoma include doxorubicin, cisplatin, and paclitaxel.
b) Hormone Therapy: Hormone therapy is a treatment that uses drugs to block or lower the levels of certain hormones in the body. This treatment is used for some types of uterine sarcoma that are hormone-sensitive. Hormone therapy can include drugs like tamoxifen or aromatase inhibitors.
Surgery:
a) Hysterectomy: The most common surgery for uterine sarcoma is a hysterectomy, which removes the uterus and possibly other nearby organs or tissues, depending on the stage and location of the cancer.
b) Lymphadenectomy: Lymphadenectomy is the removal of lymph nodes in the pelvic and abdominal area to determine the spread of cancer.
c) Debulking surgery: Debulking surgery is the removal of as much of the tumor as possible. This is usually done in advanced-stage cancer.
Radiation Therapy
X-rays and other forms of high-energy radiation are used in radiation therapy to kill or stop the growth cell cancer cells. It is often combined with chemotherapy, surgery, or both. can undergo radiotherapy.
Externally, called external radiation therapy, or internally, called brachytherapy.
Targeted Therapy
Targeted therapy is a form of cancer treatment that specifically targets certain proteins or support supports the development and spread of cancer cells.
It may be used for some types of uterine sarcoma that have specific genetic mutations. Targeted therapy drugs used for uterine sarcoma include pazopanib and trabectedin.
Immunotherapy
Immunotherapy is a type of cancer treatment that stimulates the immune system to attack cancer cells. It may be used for some types of uterine sarcoma, although research is still ongoing. Immunotherapy drugs used for uterine sarcoma include pembrolizumab and nivolumab.
Palliative Care
Palliative care is specialized medical care focused on improving the quality of life of critically ill patients. It may be used to manage symptoms, provide pain relief, and offer emotional and spiritual support for patients with advanced uterine sarcoma who are no longer responding to treatment.
It is crucial to remember that as new research and technological developments are made, uterine sarcoma treatment choices are always changing. Therefore, it is important to work closely with doctors who specialize in treating uterine sarcoma to determine the best course of treatment for each patient.
Stronger than sarcoma, Let's empower women against uterine cancer.
















